Cholerhiasis: Symptoms, Causes, Diagnosis, Treatment, and Prevention Guide
Cholerhiasis is a complex hepatobiliary condition that continues to generate clinical attention due to its diagnostic nuance, symptom overlap with other biliary disorders, and evolving treatment pathways. Although often discussed alongside gallstone disease and bile duct obstruction syndromes, cholerhiasis carries distinct pathological and management considerations that healthcare professionals and informed patients must understand.
This comprehensive authority guide explores cholerhiasis from foundational biology to advanced therapeutic innovation. It is designed to bridge medical expertise with accessible explanation—delivering clarity on symptoms, causes, risk patterns, diagnostics, treatments, and long‑term prevention strategies.
Understanding Cholerhiasis
Cholerhiasis refers to the formation or presence of calculi or obstructive material within bile pathways, affecting bile flow between the liver, gallbladder, and small intestine. The condition disrupts digestive chemistry, particularly fat emulsification and toxin elimination.
While often confused with cholelithiasis, cholerhiasis encompasses broader biliary obstruction dynamics, including intrahepatic and extrahepatic bile flow impairment. This distinction shapes both diagnosis and treatment planning.
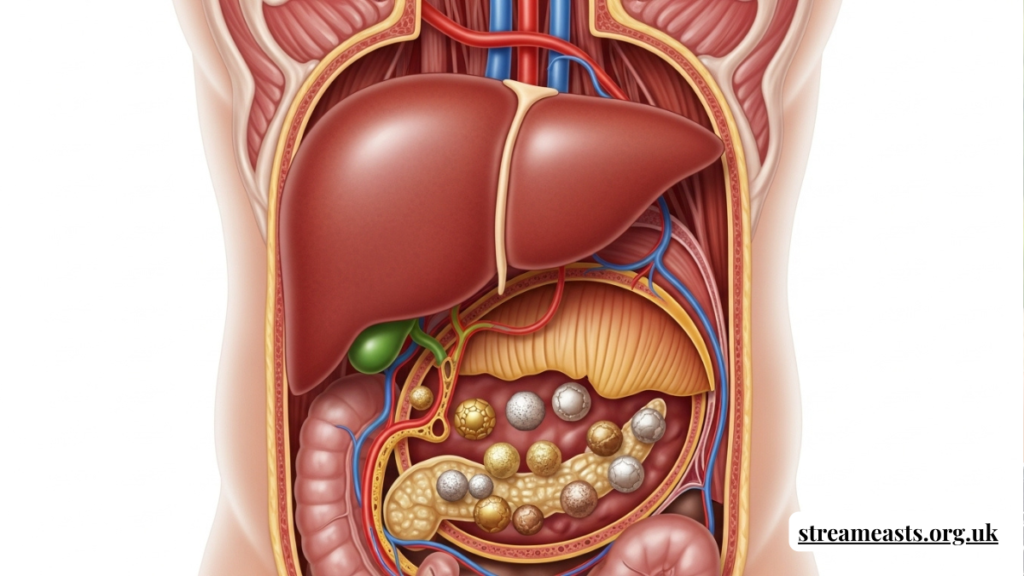
Biliary System Anatomy and Function
The biliary system is a transport network responsible for bile synthesis, storage, and release. The liver produces bile, the gallbladder concentrates it, and ducts deliver it into the duodenum during digestion.
In cholerhiasis, obstruction alters pressure gradients within this system. The resulting bile stasis can trigger inflammation, infection, or secondary hepatic stress.
Pathophysiology Behind Cholerhiasis
Choler hiasis develops when bile composition becomes imbalanced. Excess cholesterol, bilirubin, or calcium salts crystallize and aggregate into obstructive formations.
Motility dysfunction also contributes. When bile fails to circulate efficiently, sediment accumulates, accelerating calculi development and ductal blockage.
Primary Causes and Etiological Drivers
Multiple biological triggers underlie choler hiasis onset. Metabolic disorders, liver disease, and chronic inflammation alter bile chemistry and secretion dynamics.
Genetic predisposition and hormonal influences—particularly estrogen fluctuations—can further modify biliary composition, elevating obstruction risk.
Risk Factors and Vulnerable Populations
Certain demographics exhibit higher cholerhiasis incidence. Individuals with obesity, diabetes, or rapid weight loss histories face elevated susceptibility.
Age also plays a role. Biliary motility and enzymatic balance decline over time, creating favorable conditions for calculi formation.
Symptom Presentation and Clinical Indicators
Cholerhiasis symptoms range from mild digestive discomfort to severe hepatobiliary crises. Common early signs include bloating, nausea, and right upper quadrant pain.
Advanced obstruction may produce jaundice, fever, clay‑colored stools, and dark urine—signals requiring urgent evaluation.
Pain Patterns and Biliary Colic
Pain associated with choler hiasis often follows fatty meals. Biliary contractions force bile against obstructions, triggering sharp episodic discomfort.
These attacks may radiate to the back or shoulder, complicating differential diagnosis with cardiac or musculoskeletal conditions.
Digestive Disruption and Nutrient Absorption
Bile is essential for lipid digestion. In choler hiasis, impaired bile delivery compromises fat breakdown and absorption.
Patients may experience steatorrhea, vitamin deficiencies, and unexplained weight fluctuations due to chronic malabsorption.
Inflammatory Complications
Obstruction frequently initiates inflammatory cascades. Cholangitis and cholecystitis can emerge when bacteria proliferate in stagnant bile.
These complications elevate systemic infection risk, making early detection of cholerhiasis clinically critical.
Diagnostic Evaluation Pathways
Diagnosing cholerhiasis requires layered imaging and laboratory analysis. Physicians begin with symptom history and liver function testing.
Elevated bilirubin and alkaline phosphatase levels often signal biliary obstruction requiring deeper imaging assessment.
Ultrasound Imaging Insights
Ultrasound serves as the frontline diagnostic tool for choler hiasis. It visualizes duct dilation, gallbladder stones, and bile flow irregularities.
Its noninvasive nature makes it ideal for initial screening and follow‑up monitoring.
Advanced Imaging Modalities
When ultrasound findings are inconclusive, MRCP and CT scans provide high‑resolution biliary mapping. These tools detect micro‑obstructions and anatomical anomalies.
Endoscopic ultrasound adds further precision, particularly in complex choler hiasis presentations.
ERCP in Diagnosis and Treatment
Endoscopic Retrograde Cholangiopancreatography plays a dual role. It confirms cholerhiasis while enabling immediate stone extraction.
This combination of imaging and intervention reduces procedural redundancy and accelerates symptom relief.
Laboratory Biomarkers
Blood panels support choler hiasis diagnosis through inflammatory markers and hepatic enzyme profiling. Elevated AST, ALT, and GGT levels indicate biliary strain.
White blood cell elevation may signal secondary infection requiring urgent treatment.
Comparative Diagnostic Tools Table
| Diagnostic Tool | Invasiveness | Accuracy Level | Primary Use | Limitations |
| Ultrasound | Noninvasive | Moderate | Initial screening | Operator dependent |
| MRCP | Noninvasive | High | Duct visualization | Cost, availability |
| CT Scan | Noninvasive | Moderate‑High | Structural mapping | Radiation exposure |
| ERCP | Invasive | Very High | Diagnosis + treatment | Procedure risks |
| Endoscopic Ultrasound | Minimally invasive | Very High | Micro‑stone detection | Specialist required |
This comparison highlights the layered diagnostic strategy used in confirming cholerhiasis.
Treatment Strategy Overview
Treatment for cholerhiasis depends on obstruction severity, infection presence, and patient comorbidities. Mild cases may respond to medication.
Severe obstruction often necessitates endoscopic or surgical intervention.
Pharmacological Management
Ursodeoxycholic acid may dissolve cholesterol‑based obstructions in select cholerhiasis patients. It modifies bile composition to reduce crystallization.
Antibiotics are prescribed when infection accompanies obstruction.
Endoscopic Stone Removal
ERCP‑guided extraction remains a frontline interventional therapy. Instruments capture and remove ductal calculi.
This minimally invasive approach often eliminates the need for open surgery.
Surgical Intervention Pathways
When recurrence or anatomical dysfunction persists, cholecystectomy may be recommended. Removing the gallbladder prevents future obstruction.
Complex choler hiasis cases involving intrahepatic ducts may require advanced hepatobiliary surgery.
Post‑Treatment Recovery
Recovery timelines vary by intervention type. Endoscopic procedures allow rapid discharge and minimal downtime.
Surgical patients require longer healing periods but often achieve permanent symptom resolution.
Dietary Management After Diagnosis
Nutrition plays a central role in managing cholerhiasis recurrence risk. Low‑fat diets reduce biliary stimulation and pressure.
Fiber‑rich foods support digestive balance and bile acid metabolism.
Lifestyle Modifications
Weight stabilization is essential. Rapid fat loss increases bile cholesterol saturation.
Regular physical activity enhances metabolic regulation and biliary motility.
Preventive Healthcare Screening
Routine liver function testing aids early choler hiasis detection in high‑risk populations. Preventive imaging may be recommended.
Early monitoring reduces emergency intervention likelihood.
Pediatric and Rare Presentations
Though uncommon, choler hiasis can affect pediatric patients, often linked to genetic or metabolic disorders.
Diagnosis in children requires specialized imaging and tailored treatment protocols.
Geriatric Considerations
Older adults face higher complication risks due to comorbidities and delayed symptom recognition.
Minimally invasive treatment strategies are prioritized in geriatric cholerhiasis care.
Pregnancy and Hormonal Influence
Hormonal shifts during pregnancy alter bile viscosity and gallbladder motility. This can precipitate choler hiasis episodes.
Management emphasizes noninvasive monitoring unless complications arise.
Misconceptions and Diagnostic Confusion
Choler hiasis is frequently misidentified as acid reflux or peptic disease due to overlapping symptoms.
Accurate imaging differentiates biliary obstruction from gastrointestinal inflammation.
Psychological Impact of Chronic Biliary Disease
Recurrent pain and dietary restriction can affect mental wellbeing. Anxiety surrounding attacks is common.
Holistic choler hiasis care includes psychological reassurance and lifestyle coaching.
Economic Burden and Healthcare Utilization
Hospital admissions, imaging, and surgery contribute to the financial impact of choler hiasis.
Preventive care and early treatment significantly reduce long‑term healthcare costs.
Technological Innovation in Treatment
Laser lithotripsy and robotic biliary surgery are advancing cholerhiasis treatment precision.
These technologies reduce recovery time and procedural trauma.
Future Research and Clinical Trials
Ongoing research explores bile acid modulators and gene‑linked therapies for cholerhiasis prevention.
Precision medicine may soon tailor treatment to individual bile chemistry profiles.
Quote Supporting Clinical Perspective
“Biliary diseases demand early imaging, not delayed interpretation.”
This clinical principle underscores why timely cholerhiasis diagnosis improves outcomes dramatically.
Long‑Term Prognosis
With appropriate treatment, cholerhiasis prognosis is highly favorable. Recurrence risk declines after definitive intervention.
Lifestyle adherence further enhances long‑term hepatobiliary health.
Conclusion
Choler hiasis represents more than a mechanical obstruction—it is a metabolic, inflammatory, and systemic hepatobiliary disorder requiring integrated care. From imaging innovation to dietary management, modern medicine offers highly effective pathways for diagnosis and treatment.
As awareness expands and preventive strategies improve, patients and clinicians alike are better equipped to manage choler hiasis proactively—transforming what was once an acute surgical crisis into a controllable digestive condition.
FAQ
What is cholerhiasis?
Cholerhiasis is a biliary obstruction condition involving calculi or blockages that impair bile flow and digestion.
What causes cholerhiasis?
Cholerhiasis develops from bile composition imbalance, metabolic disorders, and ductal motility dysfunction.
How is cholerhiasis diagnosed?
Cholerhiasis diagnosis involves imaging such as ultrasound, MRCP, and ERCP alongside liver function testing.
Can cholerhiasis be treated without surgery?
Yes, mild cholerhiasis cases may respond to medication or endoscopic stone removal procedures.
Is cholerhiasis preventable?
Diet, weight management, and routine screening reduce cholerhiasis risk significantly.